News - Where Innovation Meets Medicine Dual Accreditation in Nuclear Medicine and Radiology
←
→
Page content transcription
If your browser does not render page correctly, please read the page content below
news
VO L . 5 1 N O . 7 | J U LY 2 0 1 9 | M C I ( P ) 0 8 3 / 1 2 / 2 0 1 8
Where Innovation
Meets Medicine
Dual Accreditation
in Nuclear Medicine
and Radiologynews
CON T E N T S
Vol. 51 No. 7 2019
EDITORIAL
BOARD
Editorial
04 The Editors' Musings
Editor
Dr Tan Yia Swam and Dr Jipson Quah
Dr Tan Yia Swam
Deputy Editors
Dr Tina Tan
Dr Tan Tze Lee Feature
Editorial Advisors
05 Radiology in Singapore –
A/Prof Daniel Fung Where Innovation Meets Medicine
A/Prof Cuthbert Teo Dr Lim Chee Yeong, Dr Xie Wan Ying
Dr Toh Han Chong and Dr Tan Bien Soo
Members
Dr Chie Zhi Ying
Dr Jipson Quah President’s Forum Doctors in Training
Dr Jonathan Tan
Dr Jimmy Teo 08 Dreams and Ruminations 18 Two Months in Fiji:
Dr Alex Wong Dr Lee Yik Voon My WHO Internship
Dr Ivan Low
EX-OFFICIOS
Dr Lee Yik Voon
Dr Lim Kheng Choon
Council News 20 Growth as a Physician
10 Highlights from the Dr Nigel Fong
EDITORIAL Honorary Secretary
OFFICE Dr Lim Kheng Choon 22 New Challenges Await New Doctors
Senior Manager Dr Benny Loo and Dr Lee Pheng Soon
Sarah Lim
Assistant Manager Reflections
Sylvia Thay 11 An Insider's Take From the Heart
Editorial Executive on Radiology 24 Celebrating Our Little Fighters –
Jo-Ann Teo Dr Chan Wan Ying, Dr Jonathan Sng Paediatric Brain and Solid Tumour
and Dr Sonia Lee Awareness Day 2019
ADVERTISING AND
PARTNERSHIP
Lau Kin Mun and Candy Tan
Li Li Loy
Tel: (65) 6540 9174
Email: adv@sma.org.sg
AIC Says
PUBLISHER 28 Practising Self-Care with
Singapore Medical Association Respite Care
2985 Jalan Bukit Merah
#02-2C, SMF Building
Agency for Integrated Care
Singapore 159457
Tel: (65) 6223 1264
Fax: (65) 6252 9693 Opinion
Email: news@sma.org.sg 14 The Roads Both Taken: Calendar
URL: https://www.sma.org.sg
Dual Accreditation in Nuclear 29 SMA Events Aug–Oct 2019
UEN No.: S61SS0168E
Medicine and Radiology
DESIGN AGENCY Dr Peh Wee Ming
Oxygen Studio Designs Pte Ltd Indulge
PRINTER
16 The Invisible Force 30 Guess the Flower
Sun Rise Printing & Dr Siva Subramaniam Dr Lynette Teo
Supplies Pte Ltd
Opinions expressed in SMA News reflect the
views of the individual authors, and do not
necessarily represent those of the editorial
board of SMA News or the Singapore Medical
Association (SMA), unless this is clearly
specified. SMA does not, and cannot, accept
any responsibility for the veracity, accuracy
or completeness of any statement, opinion or
advice contained in the text or advertisements
published in SMA News. Advertisements of
products and services that appear in SMA News
do not imply endorsement for the products
and services by SMA. All material appearing
in SMA News may not be reproduced on any
platform including electronic or in print, or
transmitted by any means, in whole or in part,
without the prior written permission of the
Editor of SMA News. Requests for reproduction
should be directed to the SMA News editorial
office. Written permission must also be
obtained before any part of SMA News is stored
in any retrieval system of any nature.editorial
Tan Yia Swam For this special "Doctors in
Training" issue, we feature the
Jipson Quah
field of roentgenology – better
Editor known as radiology these Guest Editor
days. In 1895, Wilhelm Conrad
Dr Tan is learning new skills and Roentgen was a professor of Dr Quah is in private practice as a GP
stretching new boundaries in her private physics at the University of with a special interest in pathology.
practice. Meanwhile, she still juggles Würzburg when he made his He enjoys discussing pathology
the commitments of being a doctor, greatest discovery: X-rays (also reports with patients, music-making,
a wife, the SMA News Editor, the Vice- known as Roentgen rays). He fitness and editorial work.
President of the SMA and a mother of noticed that, as a cathode-ray
three. She also tries to keep time aside for tube was being operated in a
herself and friends, both old and new. darkened room, paper lined with important paper on obstetrical
barium platinocyanide lying and gynaecological sonography.
some distance from the tube “lit It contained illustrations of
My surgical work is closely up with brilliant fluorescence”. B-mode sonograms of various
intertwined with radiology. During normal and pathological
the training years, one learnt how to Rontgen theorised that abdominal conditions, while
read CT scans and arrange urgent unknown radiation was formed also discussing the safety of
vascular interventions. Being able to when electrons struck the diagnostic ultrasound. The
have valuable discussions with like- wall of the cathode-ray tube, diagnostic ultrasound has since
giving rise to a fluorescent become an indispensable tool
minded radiologists to truly “correlate
chemical reaction. He found for obstetricians, surgeons and
clinically” was a joy. What do we
that it affected photographic emergency physicians, facilitating
make of the non-enhancement?
plates and he took the first more accurate and efficient
How about these tiny locules of air?
photographs of metal objects management of patients.
Now, doing pure breast work, and the bones in his wife’s hand.
being able to work with dedicated Unsurprisingly, the study of The dynamic field of radiology
breast radiologists is another great physics and radiation has always has been largely defined by
joy. We’d review mammograms featured prominently in the technological innovations
together (which cluster of training of a roentgenologist. combined with groundbreaking
microcalcifications should we aim clinical applications; this has
Another radiologist, given rise to rapidly advancing
for?), decide on which modality to Sven Ivar Seldinger, introduced
use next (if necessary, supplementary subspecialties, such as
the eponymous Seldinger interventional radiology, nuclear
ultrasound or MRI?), and discuss technique, a key procedural
the technique and accuracy of medicine and now, even artificial
innovation for the insertion of intelligence. I believe that all of
localisation and peri-operative chest drains, central venous us will agree that it is impossible
marking; such joint management catheters, pacemaker leads, to practise medicine without the
gives patients a better outcome. etc. The groundbreaking fine services of our radiology
It is, therefore, my pleasure to focus technique revolutionised colleagues and we are delighted
this July issue on radiology. We have angiography, which had a high to have senior and junior
invited various writers across different rate of complications back then, radiologists from the various
institutions and subspecialties to and set the foundations for healthcare institutions share their
share the recent developments and interventional radiography. insights in this issue. I trust that
progress in radiology, as well as the Ian Donald, Professor the rest of the medical fraternity
training woes and rewards. Enjoy! of Midwifery, published an will have a fascinating read.
04 JUl 2019 SMA NewsFEATURE
RADIOLOGY IN SINGAPORE
WHERE INNOVATION MEETS MEDICINE Text by Dr Lim Chee Yeong, Dr Xie Wan Ying and Dr Tan Bien Soo
Photo by SingHealth Diagnostic Radiology Residency Programme
Technological advancements are in Singapore, translating to 19.4 and volume-based model. In 2013, the
relentless in the modern era and few 14.3 units per million population, American College of Radiology
medical specialties have embraced respectively. The ratios are mid-range published their influential strategic
innovations quite like radiology. when compared to developed nations blueprint, Imaging 3.0, setting the
From the emergence of MRI to in the Asia-Pacific, Europe and North stage for the next phase of radiology
early ventures towards artificial America, which ranges from 7.4 to 97.3 targeting optimal imaging care.3 This
intelligence (AI), continual disruptive CT units and 5.6 to 43.1 MRI units per initiative comprises active radiology
evolution renders the specialty million population.2 The modalities involvement in managing imaging
abstruse to patients and professional may work in union too; for example, appropriateness, clinical decision
contemporaries alike. To understand fusion of real time ultrasound with CT support, safety, quality and providing
the essence amid such vicissitudes, for hepatic interventions or combining patient-centric care. The goal is to
we will have to connect the dots anatomical information from CT acquire the right, personalised and best
of recent key advances along or MRI with functional analysis in imaging for each individual.
the journey towards the cutting positron emission tomography (PET) These paradigm shifts in mindset
edge. This article will focus on the CT/MRI. 3D printing has also recently have brought forth changes to the
ongoing transformation of clinical created much excitement in the daily practice of a typical radiologist. A
practice in radiology, the growth of field due to technical breakthroughs typical workday begins with a clinical
interventional radiology and nuclear and decreasing cost. The models radiology round where radiologists and
medicine, as well as opportunities in generated from radiology images other clinicians from various disciplines
digital informatics. are used to optimise pre-operative get the opportunity to work together
planning across many disciplines, such by reviewing images and pertinent
Transformation of as orthopaedics and vascular surgery. clinical information to optimise patient
clinical practice management. Strides are being made
Most radiology centres in in enhancing the effectiveness of the
Since the first X-ray department began Singapore now provide subspecialised radiology report, trending towards
in the new Singapore General Hospital services, employing consultant standardised structured reporting.
(SGH) within the historic Bowyer radiologists specialising in Scoring systems such as BI-RADS
Block in 1926, radiology has grown specific interest domains such as (Breast Imaging-Reporting and Data
tremendously in scope and clinical cardiothoracic, abdominal, neurology, Systems) and LI-RADS (Liver Imaging-
impact.1 Within a century, that nascent head and neck, musculoskeletal, Reporting and Data Systems) are
single modality general practice has breast, emergency, vascular, now in practical application, using
metamorphosed into today’s multi- intervention and nuclear medicine. consistent terminology to reduce
modality subspecialty-based practice The conventional imagery of a solo imaging interpretation variability and
in all hospitals in Singapore. radiologist enclosed in the dark errors, enhancing communication with
The radiology departments today reading room churning out endless fellow clinicians and facilitating quality
provide a wide variety of imaging radiology reports in front of a blue assurance and research. Many centres
techniques such as radiography, CT, screen has become irrelevant and have concurrently introduced new-
MRI, ultrasound and nuclear medicine superseded by progressive radiologist wave integrated multimedia reports,
imaging under one roof. Local data clinician teams. Globally, radiology enabling educated patients of today to
from 2015 revealed 106 units of CT has pivoted towards a value-driven better understand their own radiology
scanners and 78 units of MRI scanners ethos, departing from the traditional report findings.
JUL 2019 SMA News 05Growth of interventional articular injections and bone tumour are now used as diagnostic criteria
radiology cementoplasty under musculoskeletal biomarkers in dementia with Lewy
intervention, as well as breast biopsy bodies and amyloid.
Interventional radiology is a specialty
with wire localisation under breast The growth in theragnostics has
well positioned to lead radiology intervention, also play integral roles in
towards value-centric goals, extending been exponential in the past decade
various clinical pathways. with the advent of personalised
our roles beyond diagnostics. It
involves utilising minimally invasive The impact of interventional medicine and therapy. Some of these
image-guided procedures to diagnose radiology in medicine today cannot newer therapies include 90 Y selective
and treat diseases in every organ be understated. For example, internal radiation therapy (SIRT)
system. By using the least invasive 24-hour emergency embolisation for hepatic malignancies, peptide
techniques available, risk to patients for management of pelvic trauma- receptor radionuclide therapy (PRRT)
is minimised and health outcomes related haemorrhage is now standard for neuroendocrine cancers and
are improved. These procedures have of care within all our major trauma prostate specific membrane antigen
less risk, pain and recovery time in centres. Interventional radiology radioligand therapy (PSMA RLT) for
comparison to open surgery. residency has become one of the metastatic castrate resistant prostate
most competitive medical specialties cancers. In 90 Y SIRT treatment of
The story of interventional radiology in the US and is poised to remain hepatomas, super-selective intra-
in Singapore began as early as 1959 so in the near future. While local arterial targeting improves tumoricidal
when Dr Chow Khuen Wai introduced residency programmes currently do radiation doses delivered to the
the Seldinger technique of vascular not offer a dedicated interventional tumour within a minimally invasive
catheterisation after returning from track at the moment, we have procedure, significantly improving
advanced training in the UK.4 Today, definitely noticed its increasing patient outcomes. SGH is also one
every radiology department within popularity among our graduating of the pioneers in introducing PRRT
local academic centres and most major radiology senior residents as their and PSMA RLT in South East Asia,
private imaging practices provide eventual choice of specialisation. attracting up to 40 referrals annually
dedicated interventional radiology from neighbouring countries, as well as
services around the clock. For example, Nuclear medicine, molecular China and Taiwan for PRRT alone.
the largest interventional radiology imaging and theragnostics Given the unique position of
service within SGH developed into
Nuclear medicine, as a specialty, grew nuclear medicine straddling expertise
a full-fledged clinical department in
out of the Therapeutic Radiology between imaging and medical
2017. Armed with eight interventional
Department and became an therapeutics, its main local specialist
radiology suites and 17 interventional
independent Department of Nuclear training programme is now a senior
radiologists, it performs more than
Medicine, SGH, in 1980. Over the years, residency programme under the Joint
10,000 procedures per year.
nuclear medicine centres have also Committee on Specialist Training,
The indications, frequency and been set up in other public hospitals accepting trainees from both internal
variety of procedures performed and private institutions to meet medicine and diagnostic radiology
in the interventional suite increase the increasing demand for nuclear residency tracks. The specialty also
steadily year after year. Procedures medicine services. has training pathways for dual
are broadly divided into endovascular From the 1980s to 1990s, accreditation in nuclear medicine and
and non-vascular methods, but majority of the imaging work radiology, equipping residents with
interventional radiologists in Singapore centred on Technetium-99m essential skills required for the exciting
are slowly but surely moving into super (Tc-99m) radiopharmaceuticals future in functional imaging and
subspecialisation based on systems. and radioiodine (I-131) therapy targeted molecular therapy.
Neurointervention has, over the last for thyroid conditions. The
decade, evolved into the first treatment discovery of accumulation of Digital informatics
of choice for hyperacute strokes and 18F-fluorodeoxyglucose (18 F-FDG) in A major inflection point for radiology
cerebral aneurysms, improving patient tumours revolutionised PET imaging was the introduction of picture
prognosis through intravascular in 1980. 18F-FDG PET was soon archiving and communication
thrombectomy and coil embolisation, established as a routine imaging system (PACS) before the turn of the
respectively. Similarly, in appropriate tracer in neuroimaging and cancer millennium. As the
patients, vascular intervention has diagnosis and management. Today, world accelerated
enabled definitive treatment of aortic 18
F-FDG remains the workhorse of towards the
aneurysms and peripheral vascular PET imaging, although there are computer age,
disease through endovascular stenting newer, more specific radiotracers our pioneers
and angioplasty. Percutaneous which have gained interest due
biopsies, radiofrequency ablations to their clinical applications
and radioembolisation of visceral in neurology, neuro-oncology 1
neoplasms by abdominal intervention and oncology. For example, 18
increased treatment permutations F-fluoroethyl-L-tyrosine (18 F-FET)
and improved quality of life in many is a promising biomarker for
oncologic patients. Vertebroplasties response assessment in gliomas; 123
for spine fractures, ultrasound-guided I-ioflupane and 18F-Flutemetamol
06 JUL 2019 SMA Newsreadily embraced new technology, of AI-augmented radiology practice. References
transiting images away from printed The lamentable regret from the 1. Chow KW. Reflections of a septuagenarian -
form onto digital screens. The impact introduction of PACS is the unwanted radiology: past, present and future. Ann Acad
was exponential. Rapid scrolling effect of radiologists retreating deeper Med Singapore 2004; 33(5):671-5.
of multiple images in digital form into the dark room, losing invaluable 2. Cheng Tim-Ee L, Sng LH, Lim CCT, Tan BS.
rapport with other clinical colleagues Imaging in the Lion City: Singapore Radiology
enabled more complex cross-sectional Country Report. Journal of Global Radiology
imaging to be obtained and optimised and patients. In an ironic twist, thought 2016; 2.
with innumerable post-processing leaders now believe that as AI/ML
3. Ellenbogen PH. Imaging 3.0: what is it? J Am
techniques. Easy access to prior algorithms are trained to perform Coll Radiol 2013;10(4):229.
imaging data improved reporting repetitive mundane diagnostic tasks,
4. Teo TKB, Tan BS, Tay KH. A brief history of
standards and efficiency. Most radiologists will finally be able to interventional radiology in Singapore and its
significantly, the ability to review concentrate on adding value, improving current status. Biomed Imaging Interv J 2011;
high-quality images anywhere in the inter-human communications and 7(2):e13.
wards and consultation rooms on managing patients beyond mere 5. Choy G, Khalilzadeh O, Michalski M, et al.
demand contributed to ubiquitous diagnostics. There is concurrently Current Applications and Future Impact of
Machine Learning in Radiology. Radiology 2018;
application of medical imaging in potential for radiology to venture
288(2):318-28.
clinical workflows today. further into precision medicine, with
many researchers reporting early results
Fast forward to the 21st century, of combining avant-garde techniques Legend
rapid progress in AI and machine in radiogenomics and AI. 1. Modern collaborative approach to add value
learning (ML) research arising from into medical imaging
advances in computing infrastructure In Singapore, efforts towards
and deep learning techniques, such as developing our radiology AI
convoluted neural networks, promises capabilities are rapidly picking Dr Lim is a consultant
a Fourth Industrial Revolution. It is no up pace. The Radiology Artificial radiologist in SGH
Intelligence Machine Learning Department of Diagnostic
surprise that radiology is one of the Radiology specialising in
first medical specialties to take the Imaging Informatics committee
musculoskeletal imaging
leap of faith by incorporating AI into under the Singapore Radiological and interventions. He
our practice. Society was formally formed in 2017 is also the associate
to facilitate development of this programme director
AI is the branch of computer science domain within Singapore. It has of the SingHealth
devoted to creating systems to perform been working closely with different Diagnostic Radiology
tasks that ordinarily require human radiology departments, as well as Residency Programme
intelligence. ML is the subfield of AI and Secretary of
domain experts, such as the Agency Singapore Radiological
in which algorithms are trained to for Science, Technology and Research, Society Musculoskeletal
perform tasks by learning patterns to explore novel methods harnessing Imaging Subsection.
from data rather than by explicit this exciting technology clinically. The
programming. Image recognition College of Radiologists, Singapore,
within scans is of particular interest and the local radiology residency Dr Xie is a consultant
in research, translating to clinical programmes have also made nuclear medicine
applications such as automated physician with the
progressive steps to insert informatics
Department of Nuclear
fracture and bone age classification and data science into the standard Medicine and Molecular
from radiographs, pulmonary nodule training curriculum, preparing the Imaging, SGH, and has
detection on CT and cartilage defect future generation of radiologists for an interest in molecular
detection on MRI. Furthermore, AI our next iteration. imaging in oncology and
applications are not confined to neurology. She is also
the programme director
automated image detection – these Change is the only constant of the SingHealth
algorithms are starting to extend into Nuclear Medicine Senior
Radiology is a specialty that continues
other operational domains such as Residency Programme.
to improve patient care by challenging
decreasing scan acquisition times,
established mindsets, inventing
automated clinical decision support
new diagnostic and therapeutic
and scan triaging.5
techniques, and assimilating the latest Dr Tan is senior
As true clinical applications of advancements in digital technology. consultant at the
AI applications have As a medical discipline that is neither Department of Vascular
continued to grow considered new nor old, she has and Interventional
Radiology, SGH. He is the
beyond the computer chosen to advert mid-life crisis though academic chair of the
laboratory over the relentless reinvention. Although her Radiological Sciences
last few years, facile face is ever-changing, her immutable Academic Clinical
fears of machines spirit of innovation will always remain Programme at the
replacing human the pillar of strength, the northern star SingHealth Duke-NUS
and the guiding light. Like the city we Academic Centre and
radiologists have
Chair of the Division of
shifted towards a live in, work in progress is always status Radiological Sciences
more sanguine view quo since we know no other way. at SGH.
JUL 2019 SMA News 07PRESIDENT'S FORUM
Dreams and
Ruminations Text by Dr Lee Yik Voon
Moving onward! All I want to do when minds as to what is material to them doctor will do his/her best for the
I wake up every morning is to take a when things don’t turn out well? patients. That doctor of choice would
look through my patient’s eyes. have stood the reasonable test of time
Some patients come in and quote
Do we prefer to look at healthcare “Dr Google”, but you will find that the and possess qualities that the patients
through our patients’ eyes or bow like and prefer. These qualities may
context is often missing. When your
to our fraternity’s approval so that be the way he/she explains various
patients do this, it may ruffle your
we may see eye to eye with our medical conditions and steps that the
feathers. However, a good doctor will
colleagues? It’s a delicate balance, patient needs to undertake to be on
need to be patient and spend time
but one we have to tread as we are the road to recovery. Some patients
on the patient sitting in front of them
trying to make healthcare more may prefer certain doctors by the way
to make a relevant analysis in the
patient-centric. they break bad news and their use of
right context.
the right comforting demeanor.
What can patients do when they
Understanding patients
encounter alarming medical news Thinking of the future
Does this mean that we have to that appear seemingly true (eg, that
know what different patients want? We have to do our part but what
vaccinations cause autism)? Many
Do we have to know their likes and happens if we only see this as a day
laymen will choose to believe the
dislikes, their preferences on how job or an occupation to bring home
fake news and use them to challenge
they receive advice and are informed the bacon? I believe that once you are
our best effort to be true to our
on treatment choices? When we a medical doctor, you will always be
profession. When fake news spreads
have an established patient-doctor one till you retire. However, in this day
like wildfire in the public domain, it
relationship that spans a decade or and age, how many would share my
becomes very real to our patients who
more, will we always know what is view? I hear through the grapevine
may choose to believe what they hear
material to that patient? Our patients that many would disagree with me,
and read. We should strive to dispel
want their right to be heard yet they and that our younger generation of
the myths.
know they are at a disadvantage doctors may only see medicine as an
as they lack domain knowledge. I believe that our patients have to occupation and not as a profession.
Will this information asymmetry trust their personal or family doctor At the opposite end, while we
influence them to change their whom they have chosen because that try our best, our patients need to
08 JUl 2019 SMA NewsDr Lee is a GP practising
reciprocate and understand that or be replaced by robots with artificial
in Macpherson. He
we too are humans with bodily and intelligence (AI) and deep learning. is also a member of
psychological needs. Perhaps one day AI may even simulate the current National
compassion and empathy instead General Practitioner
As I move into the later part Advisory Panel. He is a
of merely having the superhuman
of my life with my cohort, I often pet lover at heart who
capability of processing mountains of
wonder who will look after the older is the proud owner of
data and quoting them accordingly. a dog, and regularly
generation of doctors when they
succumb to sickness. How will the How many of our colleagues feeds neighbourhood
community cats. He
older generation of doctors manage can see this problem and attempt
also enjoys playing
their expectations of the younger to make a change? How many can online war games and
generation of doctors and vice versa? see the problem but will only whine thinks that playing
repeatedly? How many are oblivious Pokemon Go is a good
Perhaps we need to work harder form of exercise.
and will only worry when the
to groom our children, students and
machines start to appear at our front
interns early on in life. We should instill doors to take our jobs away?
values that physicians are expected
to hold steadfast throughout our I am up now, having just woken
lifetimes. We would need to select up from a nightmare. We need to
those who have the heart and inspire really wake up and get out of our
them at a tender age so that they may comfort zone. While the Ministry
seek that calling when the time comes. of Health plans the next step
We will need to set good role models with a focus on the sustainability
for them to follow. of healthcare, and monitoring
and managing the health of the
population, our medical community
The threat of AI
should seriously think not only
What we endeavour to do may come about our future but beyond that. I
to naught if society changes and look forward to your support in the
expects all doctors to behave similarly coming months.
JUl 2019 SMA News 09council news
Report by Dr Lim Kheng Choon
Supporting student-led initiatives with them her personal journey of being
Dr Lim is the
on the editorial board of SMA News and
Honorary On 22 April 2019, SMA supported the
Secretary of later on, the SMA Council, emphasising the
workshop “Called to See Patients” by
the 60th SMA benefits that members would gain from
providing refreshments for participants.
Council. He an open feedback channel and avenue
is currently The workshop was organised by Dr Ivan
for practice resources. In addition, Dr Tan
an associate Low, who was the past president of the
also mentioned that the SMA Council’s
consultant 68th National University of Singapore
at Singapore advocacy work in light of the recent
Yong Loo Lin School of Medicine’s Medical
General Hospital.
Society, and his peers. It was conceived medico-legal cases can only continue with
shortly after they received requests from the strong support of our membership.
their M5 juniors for essential tips on how On 31 May 2019, SMA Honorary
to approach and manage important Secretary Dr Lim Kheng Choon addressed
situations as house officers (HOs). graduating students from Duke-NUS
SMA, through the SMA Doctors in Medical School (Duke-NUS). Like Dr Tan,
Training (DIT) Committee, actively Dr Lim shared about his personal journey
supports student-led initiatives that as part of the pioneer batch of Duke-NUS
promote education and collegiality. and the important role SMA plays in
Interested parties with good ideas may advocating for doctors and patients. SMA’s
approach the SMA DIT Committee at advocacy efforts in the recent medico-
dit@sma.org.sg for assistance and support. legal cases regarding consent taking and
communication of confidential medical
Connecting with local information were also highlighted.
medical graduates SMA thanks TTSH, MOH Holdings
On 22 April 2019, SMA 1st Vice President and Duke-NUS for the opportunity to
Dr Tan Yia Swam spoke to HOs posted to address their HOs and graduates to
Tan Tock Seng Hospital (TTSH). She shared showcase our work.
A big thank you to all our readers who took part in the “Play and Win: How Well
Do You Know Your SMA” pop quiz published in the May issue of SMA News.
Congratulations to Dr Yong Wei Sean for winning the lucky draw prize – A 3M LED
P1610 Polarizing Task Light (worth $299).
Dr Yong Wei Sean
SMA Member since 1995REFLECTIONS
Text by Dr Chan Wan Ying, Dr Jonathan Sng and Dr Sonia Lee
Is the transformative age of radiology already here or has it not yet
arrived? Do radiologists really dislike people? Do radiology trainees
trod a lonely life of examinations in isolation?
Many, including aspiring medical students, may hold
certain misconceptions about this dynamic and ever-advancing
specialty. SMA News has thus asked three radiologists to
each share with us a short snippet on their thoughts and
experiences. Read on to find out more.
I believe that we are witnessing the shaky ground, with sweaty palms
transformative era of radiology. The and casting a suspicious glare… on
specialty has come a long way since the normal film. The dark reading
Roentgen’s famous hand X-ray in room ended up hiding my flushed
1895. My radiology training is very face more than once.
different from my mentor’s, and his
I have come a long way since that
generation practically wrote the
first film, with more than 10,000
textbooks of radiology as we know
films under my belt in the span of
today. Especially in the last few
decades, the scope of our practice my residency. A wise person once Dr Chan Wan Ying
said: To struggle is to grow. When I is a fifth-year senior
has been expanding as rapidly resident from the
as the advancements in medical reflect on my residency, the person
SingHealth Residency
technology. who has emerged is not the same as Diagnostic Radiology
the one before. Programme. Her
In my first year, X-rays were interests are in
taught as the foundation of With artificial intelligence looking body and oncologic
radiology. Yet during my entire to be the next frontier of radiology, imaging. She can
medical school training, I have perhaps my juniors’ residencies will be found in a dark
also be vastly different from mine. reporting room
read more microscope slides than
or under a pile of
X-ray films. This is how I remember The transformative era of radiology non-fiction books.
reading my first X-ray: standing on is, to me, already here.
JUl 2019 SMA News 11What do I like about are captured for posterity as
Dr Jonathan Sng is
a senior resident in
radiology? imaging is stored forever.
his fourth year of I enjoy the rapid pace of work,
radiology training being involved in the care of many Are there any
in the National
patients with diverse conditions misconceptions?
University Health
System. He is happily and interacting with the doctors Some stereotypes about
married and enjoys caring for them. For example, it radiologists include us disliking
the depth and is challenging and exciting to people and having a relaxed work
breadth of his work. switch to discussing neuroimaging day. While it is true that our day
with a neurologist shortly after is not physically intense (apart
performing an ultrasound with from interventional radiology),
the paediatric surgeons. there is almost never a time in
which we stop thinking or are not
What do I dislike mentally engaged with the scans.
about radiology? While all specialties have a variety
We can never have an “off” day. If of personalities, radiologists as a
we are tired or pushing ourselves whole are quite friendly, although
to interpret examinations it may be true that many prefer to
faster, the mistakes we make talk to doctors rather than patients.
One of the many special things Dot Course, run by senior residents juniors’ training, and
about training in radiology is the for junior residents. We aimed to we seek to continue to
sheer number of examinations provide our juniors with a fresh improve this course and
that we take over the course of five perspective on the most effective nurture educators of
years. That’s 17 to be exact. Our 14th strategies in acing this exam in a the next generation of
examination, the FRCR 2B, is our most non-threatening environment. By radiologists.
challenging hurdle. It is incredibly doing this, we hoped to not only
tedious and expensive to prepare for, improve the overall pass rate but
and the overall pass rate averages also create a strong teaching culture
60% to 70%. That may seem pretty among residents. Dr Sonia Lee is the
reasonable, but in an average cohort current chief resident
We have recently completed our at the SingHealth
of 14 candidates, that translates to second annual run of this course, Residency Diagnostic
four friends staying behind. which has been well received by Radiology Programme
A close-knit group of us who our juniors and well supported by who is on hiatus for
our residency programme. We are maternity leave. Life
were studying together for this has acutely shifted
examination in 2017 agreed that happy to report that the overall pass
from interpreting
we would pay it forward after rate improved to 90.9% in 2018 and 256 shades of grey
clearing this hurdle. We created a 100% in 2019, hopefully in part due to satiating her very
comprehensive preparatory course to our efforts! own eat-poop-sleep
machine with her long-
simulating examination conditions, We are heartened to be able
suffering husband.
appropriately named the Little Red to make a positive impact in our
12 JUl 2019 SMA NewsOPINION
1
THE ROADS BOTH TAKEN
Dual Accreditation in Nuclear Medicine and Radiology
Text and photos by Dr Peh Wee Ming
My beginnings... of what we do – the half in diagnosis – But this transition was made easier by
is almost exactly like that of a the kindness of colleagues. I remember
Having spent four years in diagnostic
radiologist, while the other half in asking a senior, Dr Low Han Chung, to
radiology residency, deep within the
therapy is akin to that of an internist sit in my initial clinics to make sure I
dark corners of the west and away from
physician or radiation oncologist. In was not telling my patients nonsense.
people (as the running joke goes), I remember the shining examples of
my inner internist resurfaced and called fact, a second and historically dominant
pathway into nuclear medicine training classical internists like A/Prof David Ng
me back to the wards. After some and Dr Kelvin Loke, who showed me
not-so-gentle cajoling by my friend and exists and leads from internal medicine.
what it meant to do your best for
mentor Dr Khor Lih Kin, I decided to patients. And of course, the sweet, sweet
take the plunge and signed up for dual One half as clinician
nurses who made everything better.
accreditation in radiology and nuclear Unbeknown to some, Singapore General
medicine – then a new and relatively With time, I learnt to titrate thyroxine.
Hospital (SGH) Nuclear Medicine sees a
untrodden road with only three brave I relearnt how to defuse explosive
significant proportion of thyroid cancer
souls before me. In lieu of my fifth and situations in clinic, how to feel necks and
and Graves’ disease patients in Singapore hard livers in the ward, how to convey
final year in radiology, I crossed clusters for radioactive iodine (RAI) therapy.
to central Singapore to do two years of the nuances of a single elevated cancer
Armed with a measly year of HO-ship marker and how to hold the hand of a
senior residency in nuclear medicine. clinical experience, albeit one enhanced fellow human being to break bad news.
The practice of nuclear medicine is by toxic luck, I tried my best to be a
about the use of radioactive substances physician again. This was not an easy RAI has existed for decades and is the
to diagnose and treat disease. It exists transition. Instead of clearing scans and template “theranostic” compound – in
as a separate specialty from radiology X-rays, I had to run full-day clinics. Scans the context of differentiated thyroid
and is often confused with sister do not holler at you after waiting for half cancer, it tells you where the cancer
specialty radiation oncology. Part of the an hour, while hyperthyroid patients (as is and treats it at the same time. This
confusion probably arose because half theranostic concept, a portmanteau of
any endocrinologist would attest to) do.
therapy and diagnostics, has become a
buzzword in recent years and it is finding
2 expanded scope in other cancers, eg,
peptide receptor radionuclide therapy
(PRRT) in neuroendocrine tumours and
prostate-specific membrane antigen
(PSMA) therapy in prostate cancer.
These services at the cutting-edge have
been started in SGH Nuclear Medicine
and have injected a new vitality into
the clinical practice. The potential for
more receptors to target and more
cancers to treat is compelling and
awaiting realisation by the plucky.
One half as imager
The other part of nuclear medicine in
imaging has many similarities to that of
14 JUl 2019 SMA Newsdiagnostic radiology. I often tell medical of the very old and very new. For instance, The added perspective is a means of
students that five main tools exist in there is deep knowledge hidden behind immediate feedback for personal growth.
the imaging toolbox: X-ray and related the humble bone scan, stored in tomes And of course, the great theranostic
techniques, CT scan, ultrasound, MRI and journals from the 1980s. On the other promise is that what we can see, we
scan and nuclear medicine. In essence, hand, the new PET tracers coming into can also solve. How far this promise
the joy of the diagnostic imager is the mainstream use carry with them a rapidly goes and how much of it can be
same joy of diagnosis shared by the rest metamorphosing body of knowledge. applied to our Hippocratic Oaths, can
of medicine. Instead of using open ears As illustration of the currency expected be limited only by our imagination.
and a patient heart to hunt for clues in of us, my programme director and
the history, we use our eyes to look for mentor Dr Winnie Lam would regularly I am glad to be walking both roads
clinical meaning on stacks of pictures. quote papers hot off the press in her in this yellow wood, even though
it is a journey without end.
Running the operations of the presentations. These new tracers have the
imaging service is common to the potential to image hitherto inaccessible
Legend
practice of both nuclear medicine and problems plaguing humanity (eg, in
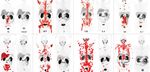
the field of dementia, we may one day 1. Society of Nuclear Medicine & Molecular
diagnostic radiology, and is a less visible Imaging’s Image of the Year 2018. Paired
aspect of our daily routine. We work image in vivo the key pathogenetic pre- and post-PSMA therapy scans
closely with allied health professionals proteins of all major syndromes). showing marked imaging and prostate-
– nuclear medicine technologists, specific antigen response in metastatic
The depth of the nuclear medicine castration-resistant prostate cancer
medical physicists and radiochemists kung fu has also been far more patients who have failed standard therapy
– to acquire the best images and profound than I had expected, with the 2. Simulated clinic encounter featuring
deliver radiopharmaceuticals safely. fundamentals drawing from different fellow colleagues on the dual-
Also common to all imaging services branches of the basic sciences compared accreditation pathway, Dr Gideon Ooi
with radiology. Knowledge of how the (left) and Dr Lenith Cheng (right)
is the need for close communication
with the rest of the clinical specialties. tracers are chemically synthesised, 3. Mini department lunch outing with
The parable of the blind men trying how they move within the body, rotating radiology residents of the SGH
Department of Nuclear Medicine and
to identify an elephant is central how they bind to target receptors, Molecular Imaging
to all aspects of the medical craft. and how the receptors are normally
Communication of what we know from expressed, are required for proper Title image and permission obtained from
our respective vantage points is required interpretation of the scan images. Prof Michael Hofman, Centre for Molecular
Imaging, Peter MacCallum Cancer Centre,
to approximate truth in each patient. Australia
The classical dichotomy of nuclear The yin and yang –
medicine is that it images functional coming together
processes, as opposed to the structural Dr Peh is currently an
Just as PET-CT is a hybrid imaging option
detail yielded by the other radiologic associate consultant
whose whole is more than the sum of its with National University
modalities. This is a division that will parts, I have found that this path of dual Hospital’s (NUH)
likely blur both ways in the foreseeable accreditation has been complementary Department of Diagnostic
future, as newer positron-emission to both my radiologist and nuclear Imaging, nuclear
tomography (PET) scanners yield medicine physician selves. On one medicine section. He
improved spatial resolution and the hand, PET-CT is like radiology with cheat serves on several tumour
other radiologic modalities gain code on, highlighting morphologically boards and contributes
improved functional capabilities. subtle and barely perceptible lesions to the diagnostic
neuroradiology and
Another dichotomy that arose in my in brilliant hues of red. On the other, nuclear cardiology
training, one that was slightly jarring, the specificity of the structural findings services. He was formerly
coming from radiology, was that nuclear limits the false-positives that come with chief resident, NUH
medicine imaging was an eclectic blend imaging ubiquitous biological processes. Diagnostic Radiology.
3
JUl 2019 SMA News 15OPINION
The X-ray that saved his life
Chest X-ray. “21/M, RTA.” It was the
second week of my first rotation in
radiology. I feel sorry for this young
man. I opened the electronic notes
from the emergency department
to find out more. He had gotten
together with his buddies for one
last night out before leaving for
university in the UK. Despite having
a few drinks too many, he decided
to drive home. Ah, the folly of youth.
Not noticing the lorry in his blind
spot, he accelerated to overtake
another car. His car hit the lorry and
went into a tailspin before hitting
the expressway divider. He’s lucky to
be alive, really. Fortunately, he walked
out of the car relatively unscathed. A
series of trauma X-rays was ordered
to confirm that there were no broken
bones. What a shame – a black mark
on his record for drunk driving! On
Text by Dr Siva Subramaniam first glance, the chest X-ray looked
normal. I methodically went through
my review areas before I spotted
the abnormality – a single subtle
undisplaced rib fracture! Good pick up!
Just as I was about to click “next”,
something caught my eye. The
16 JUl 2019 SMA Newsmediastinal contour appeared a little component, during which we have Another way in which you can
lobulated. Mediastinal haematoma? 35 minutes to diagnose 30 X-rays, help us to help you is to provide
Aortic injury? The aortic contour was with a passing mark of 90%! relevant clinical information with
normal. There was no pulmonary each request. While there are no
contusion or haemothorax. The Compassion and coffee formal statistics on this, anecdotally
findings don’t add up – better ask the most common clinical indication
Apart from examinations, night
for a CT scan. That same afternoon, for imaging across specialties is “.”.
calls are the toughest challenge
a CT chest scan was performed Clearly communicating the clinical
for radiology residents. There is a
and revealed multiple enlarged picture and your differential
constant tussle between radiology
mediastinal and hilar lymph nodes. diagnosis allows us to correctly
and other departments on call when
The patient had lymphoma. protocol the scan, titrate our
it comes to urgent scan requests. The
diagnostic sensitivity and tailor the
Moments like this are what radiology resident has to approve
report to the individual patient.
radiologists live for – picking up an every CT, MRI and ultrasound scan
incidental early cancer and saving performed while on call. As the
a life, putting disparate imaging resident on call has to report all the A new era of imaging
findings together to clinch a rare scans for the entire hospital, he/ My hope is that radiologists
diagnosis, or allaying the fears of an she must be selective in accepting and clinicians will continue to
anxious patient by giving them a scans. We try to only accept scans communicate with each other
definite answer to what’s ailing them. that are likely to affect the patient’s effectively to better understand our
management overnight. Our clinical patients’ stories and provide them
The secret lives of radiologists colleagues who request for urgent with the best of care. The story of the
scans often interpret our detailed young man with lymphoma piqued
Many people think of radiologists as cross-examination over the phone my budding interest in radiology – I
court stenographers or uninspired as a bid to block the scan. In reality, was fascinated by how the humble
journalists who simply report what we are trying to triage the scan’s chest X-ray eventually saved his
they see. It is not a glamorous job – urgency and decide whether it can life. With the advent of high-end
radiologists are rarely consulted on be performed during office hours, scanners, new imaging techniques
Grey’s Anatomy or House. Likewise, when there are more resources (CT and artificial intelligence, radiology
patients don’t see the radiologist’s and MRI scanners) and expertise is at the forefront of innovation in
role in their care – we don’t get (radiographers, sonographers and medicine. However, I believe that
many thank-you cards or cookies. consultants) available to give the these advances will augment our
To me, being a great radiologist is patient and referring team the best practice rather than replace us, and
really about being a great doctor. We possible scan and report. that radiologists will always remain
need to have a working knowledge
When we are inundated with non- at the heart of medical imaging.
of every organ system, the mental
agility of an internist and the keen urgent scans on call, we may only get Clinical correlation is advised.
instincts of a surgeon. In many ways, to read scans with critical findings
radiologists act as the invisible force much later. Furthermore, the more
scans we report, the less time we
that propels patient care across the
are able to spend on each, the more Dr Siva is Dad to
gamut of specialties.
fatigued we become and overall, the a mischievous
To equip us for this challenge, more likely we are to miss important toddler. When not
we undergo five years of rigorous findings. Imagine putting all of your child rearing, he is
training, which includes rotations a senior resident at
knowledge of anatomy, pathology,
the Department of
in diagnostic and interventional physics, pattern recognition and Radiology, Changi
radiology. Each study we report logical reasoning to the test multiple General Hospital. He
as a resident is discussed with and times a night, with only minutes has a special interest
vetted by a consultant who guides to make a critical judgement call in uninterrupted
and teaches us. Our skills are further sleep, though it
on each case. Though the physical
has been a while.
honed and tested during weekly demands of a night call in radiology
tutorials, multidisciplinary rounds are few (hey, it gets pretty cold
and, of course, examinations – which sometimes), the mental stress on
are tough and numerous. We are the resident is immense. On a busy
examined on a broad range of call, a little compassion towards the
subjects, including anatomy and radiologist can go a long way. (And
physics. Our final FRCR examination a hand-delivered cup of hot coffee
includes a rapid reporting never hurts!)
JUl 2019 SMA News 17DOCTORS IN TRAINING
2 MONTHS IN FIJI
My WH Internship
Text and photos by Dr Ivan Low
1
In medical school, we were given the headquarters for the Pacific Health Ms Nilva, a consultant from my
liberty to fill our time with any “learning Systems and Policies department of department, by the tranquil poolside.
activity” and have it count toward the Western Pacific Regional Office She pulled out a brown envelope (just
our elective programme. Some of my – one of WHO’s six regional offices like in the movies) and in it was my
friends milked cows on a farm in Japan, around the world. This meant that brief. WHO Fiji was hosting a conference
while others engaged in high-level I would be able to experience both on Pacific health information systems
research at Karolinska Institutet. But regional-level and country-level work, (HIS), and my first task as part of the
I knew I wanted to utilise the time to and get a better understanding of the Secretariat was to scribe for meetings,
explore something closer to heart. organisation’s roles and interactions with facilitate discussions, host an exhibition
various stakeholders in the complex and take photographs with my
It all started with a text message to
field that we call global health. trusty iPhone.
a public health mentor, Dr Clive Tan,
who was at that time seconded to World To answer the second question, In the weeks to follow, I had an
Health Organization (WHO) Manila. He Fiji is an archipelago-country in the abundance of opportunities to work
was immensely helpful in guiding me South Pacific approximately 2,000 on some of WHO Fiji’s projects in HIS
through the application process and kilometres northeast of New Zealand. and health service delivery. Regionally,
thanks to him, I received an acceptance It has more than 330 islands, of I helped to fine-tune and launch
letter a couple of weeks later. That was the “Healthy Islands monitoring
which two-thirds are uninhabited!
how my two-month internship with framework”, assisted in the publication
WHO Fiji began in the summer of 2016. of a Pacific HIS report, and developed
Work begins a questionnaire on health service role
Why Fiji? In the first place, where is Fiji? My first day at work was somewhat delineation policies for Pacific nations.
Master “Obi-wan” Clive had it surreal. After a ten-hour flight, I headed Locally, I was part of a team that looked
all thought out – Fiji serves as the over to the Tanoa Hotel where I met into mapping the healthcare needs of
18 JUl 2019 SMA NewsFiji’s rural Northern Division through valued my contributions, yet there was
qualitative interviews and site visits. always a comforting layer of supervision
Many people have asked me what and gentle guidance. Furthermore,
a typical day as a WHO intern was like. the team comprised individuals from a
Frankly, there was nothing sexy about diverse range of backgrounds – there
it. The day would begin at 7 am, with a were nurses, pharmacists, physicians,
45-minute crowded bus journey down statisticians, environmental scientists
to the business district. All morning I and administrators; every conversation
would be flipping references, crunching broadened my perspective on what
data or typing furiously, save for a public health (and the profession
couple of minutes spent walking to the that runs it) was, is, and can be.
pantry for rehydration and deep vein
thrombosis prophylaxis. Lunch would Other than work
be at the nearby mall with some fellow Apart from work itself, I spent a great
interns. After recharging, the afternoon deal of time exploring the capital Suva
will often be filled with meetings, and the surrounding districts. I witnessed
sometimes held at the Ministry of an environmental protection public 2
Health’s office down the road, till 6 pm. campaign at the park, trekked through
Gradually, amid the routine buzz (and subsequently got lost in) a tropical essential to understand how health
of work that surrounded me, I began rainforest that sat on the edge of the city, issues affect our communities, and
to appreciate the “WHO method”. The drank kava with the locals (and felt my know our roles in our public strategy
Organisation’s strengths lie in being a tongue and mind go all tingly), partook toward combating these challenges.
neutral broker, having strong in-country in their massive meals with gargantuan
portions of rice, and strolled down long After all, public health is much
presence, and being (relatively) well
stretches of idyllic coral-laden beaches more than just a professional career
resourced. This enabled it to carry out
its mission of providing leadership and (1-0 to me for steering clear of Vibrio or a specialised field of practice. It
setting standards for important health vulnificus). I have come to realise that this is a mindset and a way of life.
issues, providing tailored evidence-based too has strengthened my appreciation of
technical support for capacity building, sociocultural determinants of health in
Legend
monitoring and assessing health Fiji and the Pacific.
outcomes across the board, and shaping 1. Colonial War Memorial Hospital – Fiji's
Needless to say, it was an incredibly flagship hospital
the international research agenda.
illuminative experience. I think all 2. Kava – locals drink it more often than water
Being an intern in the Organisation medical students and junior doctors or wine
was indeed eye opening. The team should immerse themselves in some 3. Every Friday is Bula Shirt Friday
entrusted me with critical responsibilities form of public health exposure during
for important WHO projects that their formative years of training. Whether
addressed emerging health trends. They as a full-time clinician/radiologist/ Dr Low is currently
encouraged independent thought and pathologist/medical innovator, it is a medical officer in
Singapore General
Hospital, Block 1. He has a
3 passion for public health,
community outreach and
medical education. In
his spare time, he can be
found relaxing at the park
with his family and loved
ones, his dog and a cup of
kopi c peng (siew siew dai).
JUl 2019 SMA News 19Growth
DOCTORS IN TRAINING
AS A PHYSICIAN Text by Dr Nigel Fong
A junior doctor’s reflections on what he has learnt so far, and how much more he has to go.
I’m rarely sentimental, but recent conversations with starry-eyed 19-year-olds
considering a career in medicine (or otherwise) has made me ruminate about “old
times” as a pre-clinical student. Dr Fong is a SingHealth
Internal Medicine
As a student, it often seemed that the journey as a physician was all about
resident. He enjoys
clearing the next hurdle – passing MBBS, entering a residency of choice, passing teaching juniors and
more exams, becoming a registrar, passing even more exams, before finally exiting. medical students, and
As a house officer (HO), priorities changed. Most of us wanted to grow an hopes that his recent
book Algorithms in
extra pair of hands to cope with the never-ending admissions and incessant Differential Diagnosis
phone calls. We learnt how to keep sick patients alive till dawn and not get is helpful for future
scolded the next morning. generations of
medical students
But what truly is growth as a physician? I’ve come to realise that it is so much and house officers.
more than jumping through hoops or becoming battle-hardened.
A physician grows by…
Learning to manage
Developing clinical treatable differentials, trying uncertainty
reasoning not to diagnose motor neuron Clinical reasoning is important, but
disease, because it is such a terrible sometimes not enough. Patient cases
Clinical reasoning – not knowledge
– makes the difference between a disease. So the process of diagnostic are increasingly complex and one often
student and a seasoned medical reasoning matures from guessing,
faces acutely unwell patients with no
officer. When I teach students, I find hypothesis testing, to a combination
clear diagnosis. This makes many of us
that many can quote evidence-based of structured algorithms and
uncomfortable. But a physician grows by
treatment of heart failure, yet are unstructured intuition.
learning to manage uncertainty.
stumped when given a breathless Algorithms can be learnt and I have
patient and told to “figure out what is First is to have situational awareness.
put together some of these with the
wrong”. Many can list differentials for In a sick patient, stabilising physiology
caveat that they are not a substitute
a symptom, but struggle to interpret (airway, breathing and circulation) often
for seeing real patients. That would
what the patient in front of them says. requires little knowledge of the exact
be a tragedy, for an algorithmic
diagnosis. When there is little to lose,
One critical aspect of clinical framework without illness scripts is
multiple possibilities must be pursued
reasoning is the ability to diagnose akin to a well-organised library with
and even empirically treated in parallel.
– if one can’t diagnose, one can’t no books. Indeed, patients have
treat. Suppose a 40-year-old Conversely, in an elective setting, there
proven to be my best teachers time
lady presents with a three- and time again. ought to be some diagnostic certainty
month history of progressive before starting higher-risk treatment.
Another critical aspect of
quadriparesis. Examination finds Secondly, I have learnt to think ahead
clinical reasoning is the ability to
symmetrical weakness with wasting, and strategise how to go forward. For
fasciculations, brisk reflexes and ask the right questions – going
beyond “this patient has asthma” to example, in a patient with recent cerebral
normal sensation. A student might haemorrhage, a CT pulmonary angiogram
connect wasting to nerve or muscle “why is she having such frequent
flares?” or “is this simply asthma, is of little value, for even if a pulmonary
disease, or equate brisk reflexes embolism is diagnosed, treatment (ie,
to stroke. A resident might use an or something more?” This requires
intellectual curiosity, plus the anticoagulation) would be contraindicated.
algorithm and localise the lesion
to bilateral brain or motor neuron discipline of deliberate reflection Thirdly, I have also learnt to engage
pathology. A registrar might to extract key lessons from patients the patient (and family) to have an
immediately and intuitively recognise seen, integrate new insights with honest conversation about treatment
motor neuron disease. Finally, a existing knowledge and apply these options and their risks and benefits, and
consultant might think hard for takeaways to new patients. also to make a shared decision.
20 JUl 2019 SMA NewsYou can also read